What is anal fissure surgery?
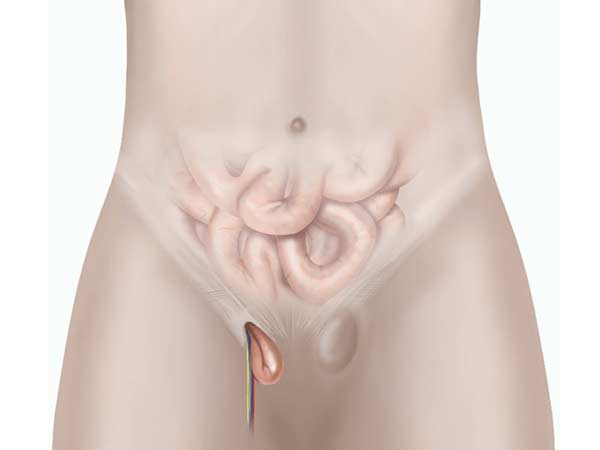
An anal fissure is a small tear in the tissue (mucosa) that lines the anus. Anal fissures often cause pain and bleeding during bowel movements. You may also feel spasms in the ring of muscle at the end of your anus (anal sphincter).
Most people with anal fissure respond to hygienic-dietary measures and pharmacological treatment, but sometimes, if there is a good response to them, they may need surgery.
Previous considerations.
Before any surgery, an assessment should be carried out by the anesthetist where they will advise you which medication you should stop taking and which you should continue taking. Sometimes you must be evaluated by another specialist if you have underlying diseases.
In the case of anticoagulant treatment or treatment that facilitates bleeding, the anesthesiologist, haematologist, cardiologist or general practitioner must inform the attitude to be followed.
In the case of smoking, the habit should be stopped because it facilitates anesthetic management, smoker patients have more complications than smokers in anesthetic procedures.
It is recommended to perform moderate-intensity exercise before any intervention, unless there is a specific contraindication, such as walking at least 60 minutes a day.
How is the preparation prior to the intervention?
FOOD AND MEDICINE
In preparation for anal fissure surgery, your surgeon may ask you to:
- Do not eat anything before surgery. You may have a sip of water with your medications, but avoid eating and drinking for at least six hours before surgery.
- Discontinue certain medications and supplements. Talk to your doctor about all medications and supplements you take. You continue to take most medications as directed by your doctor. Your doctor may ask you to stop certain medications and supplements because they can increase your risk of bleeding.
How is the surgery performed? (type of incision, resection, type of drainage, anesthesia)
BEFORE THE INTERVENTION
An anal fissure surgery can be performed under general or spinal anesthesia. Numbing medications will be given intravenously in your arm or through a catheter in your spine. Once the medications take effect, the health care team will insert a tube down your throat to help you breathe if your case ultimately benefits from a general anesthetic. Your surgeon will then perform the surgery.
DURING THE PROCEDURE
Lateral internal sphincterotomy. This technique consists of making a partial cut of the muscle fibers that form the anal sphincter, which will allow less tension to exist on the anal fissure and achieve its healing.
What happens after the surgery?
After surgery, the patient slowly awakens from the effects of the anesthetic drugs, so they may have a feeling of not remembering the process. He will spend a short period of time in an area called post-anesthetic recovery, before being taken to his room.
HOW IS THE RECOVERY IN THE HOSPITAL?
It is possible to feel nausea or abdominal pain after the intervention but they will be controlled with the prescribed medication. After about 6 hours, you will begin with the intake of liquids and then solid foods. We recommend sitting down and starting to walk about 8 hours after the intervention. You will be supervised at all times by nursing staff.
If your surgery was performed in the morning and you have no previous illnesses, you may be discharged at the end of the day. If your surgery took place in the afternoon, you will usually leave the following noon.
HOW IS THE RECOVERY AT HOME?
When you are discharged home, you will be prescribed medication so that you feel as comfortable as possible, so you will have painkillers for when you have pain. Sometimes you may need heparin injection to prevent the appearance of thrombi in your legs. You will resume your previous medication following the surgeon’s recommendations, since some drug may not be recommended in the first days after surgery.
In relation to food, we recommend a diet rich in fiber (vegetables, salads, fruit…) together with an abundant intake of water to ensure that your stools are of a soft consistency and produce the least anal pain when defecating. You may need fiber or laxatives if you have significant constipation after the intervention.
We will recommend sitz baths with warm water and neutral soap several times a day and after defecation. This will ease your discomfort. Avoid using toilet paper.
Walk every day and as you feel less pain, increase the time you dedicate to it. Avoid physical exertion until the surgeon assesses you.
Virtually full recovery can take approximately two weeks after surgery.
What are the risks of anal fissure surgery?
The normal thing is that your intervention proceeds without incidents but you must know the potential complications.
Less serious and frequent risks: Bleeding and infection of the wound, edema of the anus, water retention of urine, prolonged pain in the area of the operation.
Infrequent and serious risks: Significant infection of the perineum, incontinence to qases and even feces, stenosis of the anus, reproduction of the fissure.
death.and even feces. Anus stenosis. Reproduction of the fistula.
These complications are usually resolved with medical treatment (medications, serums, etc.), but they may require a reoperation, and in exceptional cases death may occur.
Your risk of complications depends on your overall health and the reason you’re having fistula surgery.